 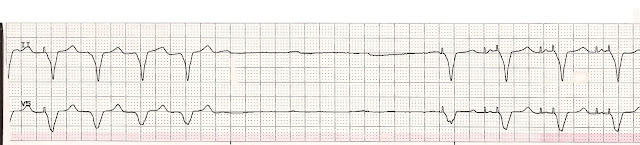 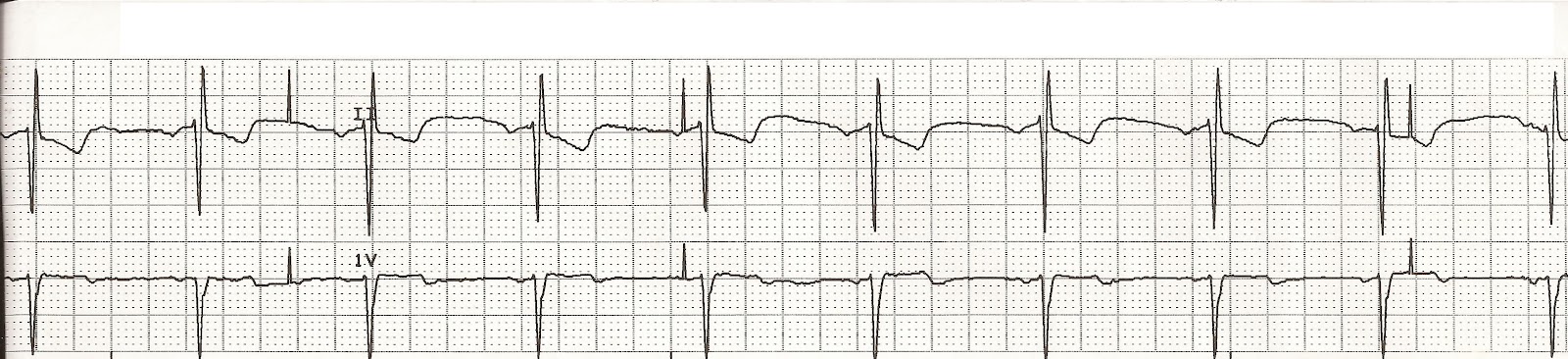
If the output energy has been reduced, the stimulus may be virtually invisible on some ECG leads or may be eliminated entirely by high-frequency filters in the recording system. However, with current digital recording systems, this distinction is no longer reliable. Historically, on analog recording systems, unipolar stimuli were large and easily visible, and bipolar stimuli were diminutive and at times difficult to recognize. To establish true noncapture, it must be determined that a pacing stimulus was present on the ECG. This is designated "functional failure to capture." While this may reflect a sensing malfunction, it is a normal phenomenon with regard to capture and should not be considered true capture malfunction. One explanation for apparent loss of capture is failure to sense a native QRS complex followed by the release of the pacing stimulus at a time when the myocardium is physiologically refractory and incapable of being stimulated. The diagnosis of loss of capture is based upon the presence of a stimulus, without a subsequent P wave or QRS complex, which occurs at a time when the myocardium is physiologically capable of being depolarized. It is differentiated from capture by the absence of an evoked potential following the pacing stimulus. The failure of that stimulus to produce electrical activation of the heart and a subsequent cardiac contraction is called noncapture or loss of capture. 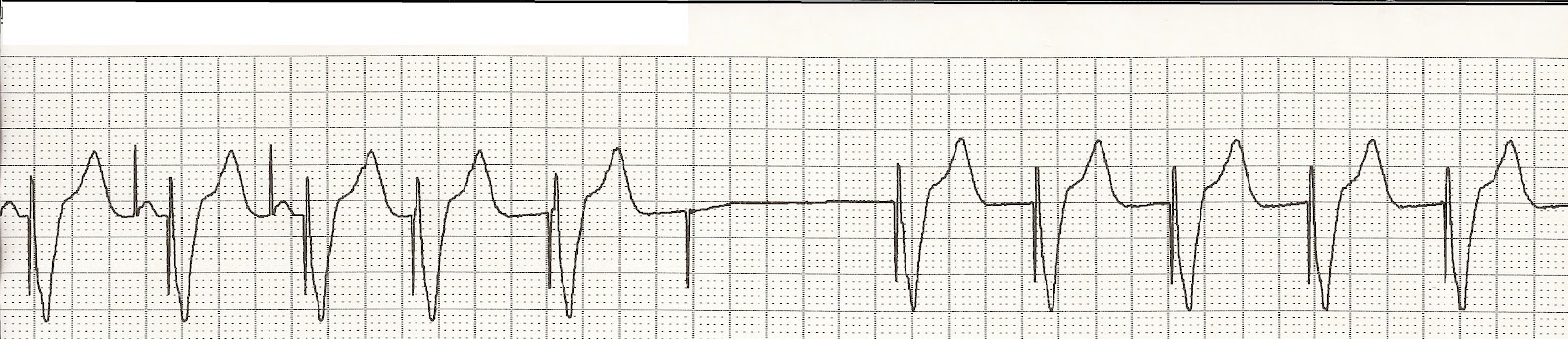
This is accomplished by the release of an output pulse or stimulus from the pacemaker that is delivered to the myocardium via the pacing lead, inducing a depolarization of either the atrium or ventricle, depending upon the location of the lead. PACING STIMULI PRESENT WITH LOSS OF CAPTURE - One of the principal requirements of a pacing system is that it prevents a heart rate that is slower than a predefined rate. As a result of a series of lead malfunctions, a policy was published by Heart Rhythm Society with lead performance guidelines. In terms of lead malfunction, more complex implantable cardioverter-defibrillator leads have a higher incidence of failure than simpler pacemaker leads. In terms of comparative reliability, there is a higher incidence of complications of leads compared with pulse generators. Overall, device hardware is highly reliable. INCIDENCE - The incidence of pacing system malfunction is difficult to determine due to inconsistent definitions and the lack of any comprehensive reporting mechanism or registry. Recording system artifacts must always be considered in the differential diagnosis of a pacing system malfunction. The normal characteristics and unique timing systems and algorithms of a given pacemaker are also an issue, as they may be interpreted as a malfunction by a clinician who is not familiar with the specific pulse generator. Inappropriately programmed pacemaker parameters, although they do not represent abnormal pacing system function, may be suboptimal for the patient. The phrase "pacing system malfunction" includes problems that might arise from any of the components of the system. PACING SYSTEM COMPONENTS - The traditional pacing system is comprised of the pulse generator ( picture 1), also called the pacemaker, and the transvenous or epicardial lead or leads that connect the pulse generator to the heart. (See "Infections involving cardiac implantable electronic devices: Epidemiology, microbiology, clinical manifestations, and diagnosis" and "Cardiac implantable electronic devices: Long-term complications", section on 'Tricuspid regurgitation' and "Dual chamber pacing system malfunctions of timing, sensing, and capture: Evaluation and management".) These include infections, venous thrombosis and emboli, pacemaker syndrome, tricuspid regurgitation, and specific problems associated with dual-chamber pacemakers. The malfunctions discussed will be limited to those that are manifest on an electrocardiogram (ECG) rhythm strip.Ĭomplications not related to pacing system malfunction - Other complications not related to pacing are presented separately. Common pacing system problems of single and dual chamber pacemakers and the methods of evaluation and therapy will be reviewed here. INTRODUCTION - Periodic evaluations of an implanted pacemaker are required to maintain optimal programming and to identify any system problem that should be corrected. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
